- Abscess Incision and Drainage
- Advancement Flap Repair
- Anal Bulking
- Anal Tattooing
- Botulinum Toxin Injection
- Colectomy
- Delorme’s Procedure
- ELAPE Procedure
- Femoral Hernia Repair
- Fistulotomy
- Haemorrhoidectomy
- HALO-RAR Procedure
- Inguinal Hernia Repair
- Intersphincteric APR
- Lateral Internal Sphincterotomy
- Low Anterior Resection
- Pelvic Organ Prolapse
- Perineal Rectosigmoidectomy
- Rectoanal Repair
- Rubber Band Ligation
- Stapled Haemorrhoidopexy
- Stoma Creation
- Stoma Reversal
- Transanal Rectocoele Repair
- Umbilical Hernia Repair
Intersphincteric APR
An intersphincteric APR (abdominoperineal resection) is an operation to remove the internal anal sphincter and rectum. It is usually performed in patients with colorectal cancer low in the rectum where the cancer does not affect the anal sphincter muscles, but where these muscles are weak and there is a high risk of severe faecal incontinence after surgery. The intersphincteric (perineal) part of this procedure may be performed in patients with severe inflammatory bowel disease (ulcerative colitis or Crohn’s disease) undergoing a panproctocolectomy (removal of the entire colon, rectum and anal canal).
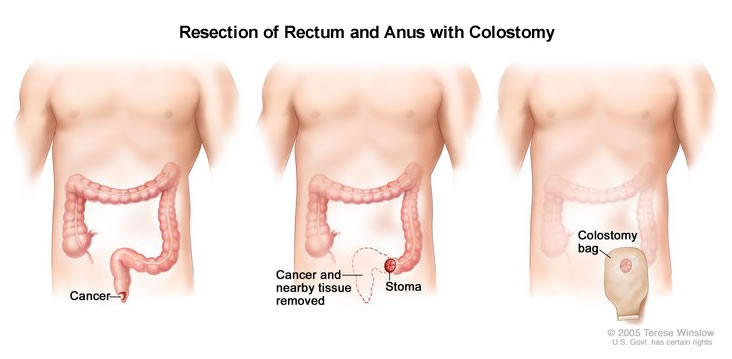
Unlike ELAPE, intersphincteric APR does not remove the anus completely along with the pelvic floor muscles. It removes the internal anal muscle as well as the bowel above and leaves the external anal muscle portion behind. However, a colostomy is required, so stoma creation is included in the procedure. The colostomy then remains in place lifelong. You will have the opportunity to discuss fully all the risks and benefits of this operation with me before signing your consent form.
If you are having this procedure to treat colorectal cancer, you may have radiotherapy or chemoradiation (chemotherapy and radiotherapy) to shrink the cancer beforehand to make the cancer easier to remove and decrease the risk of it coming back later on.
An intersphincteric APR has two parts to it, ie, an abdominal part, which is almost always planned as a minimally invasive (laparoscopic or robotic) approach, and a perineal part, which is performed using an open approach.
The abdominal part of the procedure is performed using instruments inserted through several small cuts on the lower abdomen.These cuts are about 1–1.5 cm long. A small video camera is passed through one of the cuts so that the inside of the abdomen can be seen on a TV monitor, and special surgical tools are passed through the other cuts to free the structures to be removed from the surrounding tissues. Carbon dioxide gas is used to inflate the abdomen slowly and give a clearer view of the rectum and colon. The rectum is first disconnected from the healthy sigmoid colon using a keyhole stapling device. The healthy end of the sigmoid colon is brought to the outside of the body through a larger cut (3 cm long) on the left side of the lower abdomen, and sutured to the skin, forming a colostomy. Faeces will pass through this into a stoma appliance bag. It may be necessary to put a mesh in the abdomen around the colostomy to minimise the risk of complications in the future. The other surgical wounds are closed with dissolvable stitches, followed by application of surgical glue that makes the wounds watertight.
In the perineal part of the procedure, the skin around the anus is incised and the internal and external anal sphincter muscles are separated. The internal sphincter is then removed, along with the bowel above. The remaining external anal sphincter is then simply stitched closed and no plastic surgery is needed.
The blood vessels supplying the structures that have been removed are sealed and cut by special surgical instruments via the abdomen and perineum so the amount of blood loss is minimal. A surgical drain is placed in the pelvic cavity. This is a thin tube that comes through the abdominal wall to the outside.
You will be given a long-acting antibiotic in the anaesthetic room and an injection of local anaesthetic before you leave the operating theatre. The whole procedure takes 2–4 hours to perform, depending on complexity and patient factors.
There is a 5% chance of a planned intersphincteric APR that starts as a laparoscopic procedure needing to be switched to an open one. This involves making a single long (20 cm) incision on the lower abdomen to access the rectum and using surgical tools directly to free the rectum from the surrounding tissue. Again, the procedure takes 2–4 hours, depending on complexity and patient factors. This is most likely to occur in patients who are obese and in those who are found to have an obstruction or have adhesions from previous surgery.
An intersphincteric APR is done under general anaesthesia, so you will be asleep and feel no pain. You will need to fast from midnight on the night before if your surgery is scheduled for the morning, or from 7 am if it scheduled for the afternoon. You will be given an enema an hour or so before your surgery.
After your operation
After your surgery, you will be taken to the recovery area and then to the ward. When you wake up, you will have several tubes attached to your body, including an intravenous infusion tube in your arm to give you fluids and any necessary drugs, a catheter in your bladder to drain urine, and a drain in your abdomen to remove any oozing fluid. Most or all of these tubes are removed after 24–48 hours. Supplementary oxygen is given by nasal prongs.
Some discomfort is common after this type of surgery when your local anaesthetic wears off. The anaesthetist will decide on the method of postoperative pain relief that is best for you. Oral painkillers are all that is needed in most patients, but others require intravenous analgesia or an epidural. Intravenous analgesia can be provided by a patient-controlled analgesia device, where a drip in your arm is connected to a syringe of pain-killing medication within a box. When the patient presses a button, a small dose of medication is pushed into the drip. There is a lockout that makes it impossible to overdose. When you are discharged, you will be given pain medication to take home. It is best to keep taking this medication until discomfort when going to the toilet is manageable.
You can eat and drink as you wish after the operation, and if there is no problem with drinking, the drip providing fluid will be stopped. Some patients feel a little nauseous after eating and drinking soon after their surgery. In these patients, we wait a little longer before introducing food and fluids and keep the fluid drip going. You will be mobilised on the day following your surgery. The stay in hospital after an intersphincteric APR is around 7–10 days, and sometimes a little longer. Essentially, you will be able to go home when you are confident you can manage your stoma by yourself.
Many people find that their bowel function returns to normal within about 3 days after surgery, and they can resume their normal diet at that time. Eating a balanced diet after your operation will aid your recovery. You may be given take-home medication to thicken or loosen your stools as needed.
You will not be able to drive when you are discharged from hospital, so it is important to arrange a friend or relative to take you home. When patients can resume driving after this type of surgery is determined on a case-by-case basis. This is usually 2 weeks, but will be discussed with you after your operation. Most people need longer before they can safely, forcefully, and quickly press the emergency footbrake to avoid a potential incident whilst driving. Please let your insurance company know when you have been given the all-clear to resume driving.
When you get home
Many people feel tired and weak after major surgery of this type, and full recovery may take up to 2 months. When you get home, you will need someone to help with meals, housework, and shopping. For the first week or two you may tire easily, so try to alternate short periods of light activity and rest in bed, taking care not to spend too much time lying down because of the risk of developing a blood clot in your legs (deep venous thrombosis).
Do not lift anything heavy, such as children, groceries or washing, or do strenuous work like digging the garden or lawn mowing for the first 6 weeks. You may resume intercourse when you wish.
You may get some pain off and on around your wound for several months, especially as you start to move and exercise more. This is to be expected. Taking a mild painkiller regularly will help with this. If the pain does not seem to improve or you are worried, contact your GP or our colorectal nurses.
How soon you can return to work following your surgery depends on what type of work you do, and this will be discussed with you after your operation.
A follow-up appointment in the clinic will be arranged in 1–2 weeks after your surgery to check your wounds and discuss any further management if required. If your intersphincteric APR was performed to remove a rectal cancer, the laboratory report will be discussed with you at your next appointment.

