Colonoscopy
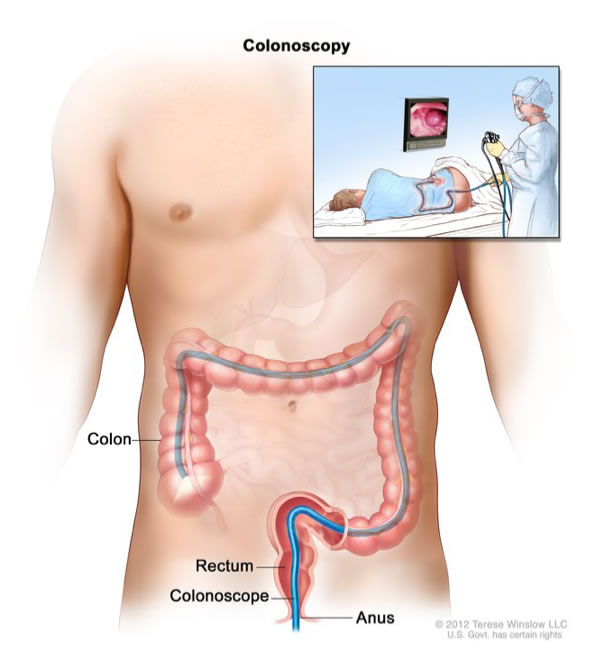
Colonoscopy is a procedure used to diagnose and treat a number of problems encountered in the colon (large bowel). It is performed using a colonoscope (a long, flexible tube about the thickness of a finger, with a tiny video camera attached to the end). The colonoscope is passed into the rectum and then moved slowly along the entire colon, while images of the lining of the colon taken by the camera are displayed on a television screen. These images are taken as the colonoscope is being inserted and again as it is being withdrawn.
A colonoscopy can help to diagnose conditions such as polyps (small benign growths of tissue projecting into the bowel), cancer, inflammatory diseases of the colon (such as Crohn’s disease and ulcerative colitis), and diverticulitis (inflammation of outpouchings that form on the walls of the colon). If an abnormal area is seen, an instrument can be passed through the colonoscope to take a small sample of tissue (biopsy) for examination in the laboratory.
Colonoscopy can also be used to remove polyps. Some polyps can become cancerous, so early detection and removal of these is important to protect against bowel cancer. If a polyp is seen during a colonoscopy, a wire loop can be passed through the colonoscope and snare the base of the polyp, which is then severed from its attachment to the bowel wall by an electric current. The procedure can also be used to re-examine the colon after a polyp or cancer has been removed to check that no new growths have occurred. Whilst I do not perform bowel screening as part of our nationwide NHS bowel cancer screening programme, I do remove polyps up to a certain size if I happen to see them while examining the bowel for another reason.
For colonoscopy to be successful, the bowel must be completely empty. This requires you to start a low-fibre diet three days before and then switch to a clear liquid diet one day before colonoscopy. You will also need to take a special laxative to clear your bowel completely on the day before your colonoscopy. You will receive detailed instructions on how to do this before your procedure. The following websites explain in detail what you can eat and drink on a low-fibre diet (www1.ghc.org/html/public/specialties/gastroenterology/colon-diet) and what drinks can be taken on a clear-liquid diet (www1.ghc.org/html/public/specialties/gastroenterology/colon-diet1).
Colonoscopy can be uncomfortable but is rarely painful, so general anaesthesia is usually not necessary. Air will be passed through the colonoscope and into the colon to make the bowel lining easier to see. When this happens, you may briefly feel pains similar to trapped wind. Often the procedure is performed with intravenous sedation, meaning that you are likely to sleep for most of the procedure. Colonoscopy may take up to an hour to perform.
If you have been sedated during the procedure, you will need to rest for two hours before going home. You must not drive for 24 hours if you have had sedation, so please arrange in advance for a relative or friend to take or accompany you home. If you have not had any sedation, you will be able to go home within half an hour and carry on with your usual activities. However, whether you have been sedated or not, we recommend that you stay for a drink and something to eat before you leave the hospital.
At the end of the procedure, the results will be discussed with you and any samples taken will be sent to the laboratory. A report is usually available shortly afterwards and a copy will be given to you and sent to your general practitioner.
Perforation of the colon is a rare but serious complication of colonoscopy where a hole is made in the bowel. It occurs in less than 0.08% of cases. The risk of perforation following colonoscopy where a polypectomy (removal of a polyp) is also performed is 0.3%–1.0%. If this happens, and the hole is small, it may settle with antibiotics, but in some cases abdominal surgery is needed to close the defect in the bowel wall. Every care is taken to avoid this complication.

